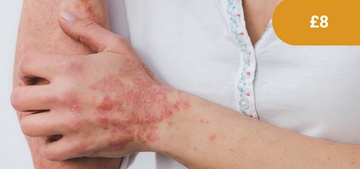
Psoriasis
GPs
Awarded with
1 CPD HOURS

Psoriasis CPD Overview
Psoriasis is an inflammatory skin disease that typically follows a relapsing and remitting course. It can occur at any age, although it is uncommon in children (0.71%) and the majority of cases occur before 35 years.
Psoriasis, for many people, results in profound functional, psychological and social morbidity, with consequent reduced levels of employment and income. Factors that contribute to this include symptoms related to the skin, problems related to treatments, psoriatic arthritis, and the effect of living with a highly visible, stigmatising skin disease. Even people with minimal involvement state that psoriasis has a major effect on their lives.
For most people, psoriasis is managed in primary care, with specialist referral being needed at some point for up to 60% of people.
Once you complete this module — and achieve the minimum pass rate of 60% — you'll be awarded with a downloadable 1 hour CPD Certificate, which you can print or upload to your CPD Portfolio.
Aims & Objectives
This module is composed of 10 assessment questions on psoriasis and has been specifically designed for GPs. On successful completion of this module, you will have an improved understanding of:
Subtypes of psoriasis and their treatment
The impact of psoriasis (e.g. disease severity and psychological/social impact)
The association of psoriasis with other conditions (e.g. arthritis, cardiovascular disease, alcohol dependence and depression)
Indications for specialist referral of psoriasis (e.g. diagnostic uncertainty, severity (>10% BSA), failure of topical agents, guttate pattern, and severe impact on physical, psychological and social well-being)
Risks and benefits of the most commonly used systemic therapies (methotrexate, ciclosporin, acitretin), their contra-indications and the need for monitoring
The role of biologic treatments in the control of psoriasis and to have an understanding of the potential risks in this patient group
Our Dermatology CPD Course
Dermatology CPD Course
10 Modules Only £20
Why StudyPRN?

Online Access
Available all year round with 24/7 online access and unlimited resits, you'll be able to learn around your busy schedule and get to grips with your CPD modules whenever you'd like — all you need is an internet connection.

Quality Assured
Our CPD modules are written and edited by medical experts within their specialist fields, who have pedigrees in postgraduate education. Questions are reviewed on a regular basis to ensure that they remain relevant and up-to-date with new guidelines.

Boosting Clinical Knowledge
As a healthcare professional it's important for you to continuously expand on your clinical knowledge, skills and abilities. Our CPD modules will help you achieve this by providing you with a full explanation of answers, further reading, and the option to reflect using our online notes system.